What are Bioactive dental materials?
Bioactive dental materials release compounds that help regenerate or maintain dental structures. In the past fluoride release was the only mineral that was in bioactive materials. Today we have materials that also release calcium and phosphate ions. Dentists use bioactive materials to remineralize dentin, repair bony defect, and maintain dental prosthetic margins
Another definition of bioactive dental materials
A bioactive dental material is something that forms a layer of hydroxyapatite or apatite like substance when immersed in saliva or a solution containing inorganic phosphate. Bioactive refers to the materials ability to induce a response from a living cell. It’s unclear if this definition excludes fluoride releasing dental materials, but I have fluoride releasing material on this page.
How do bioactive dental materials work?
Release of calcium from these materials, is what makes all of the non-flouride only bioactive materials work. This calcium works to help pulpal healing, promote immediate bonding and sealing, stimulate hydroxyl-apatite, and form secondary dentin. The material design often includes a biocompatible matrix material, bioactive molecules, or additive molecules and ions.
Why do dentists use bioactive materials?
Remineralization of dentin, repair of bony defects, and maintenance of dental prosthetic margins.
Classifications of bioactive dental materials
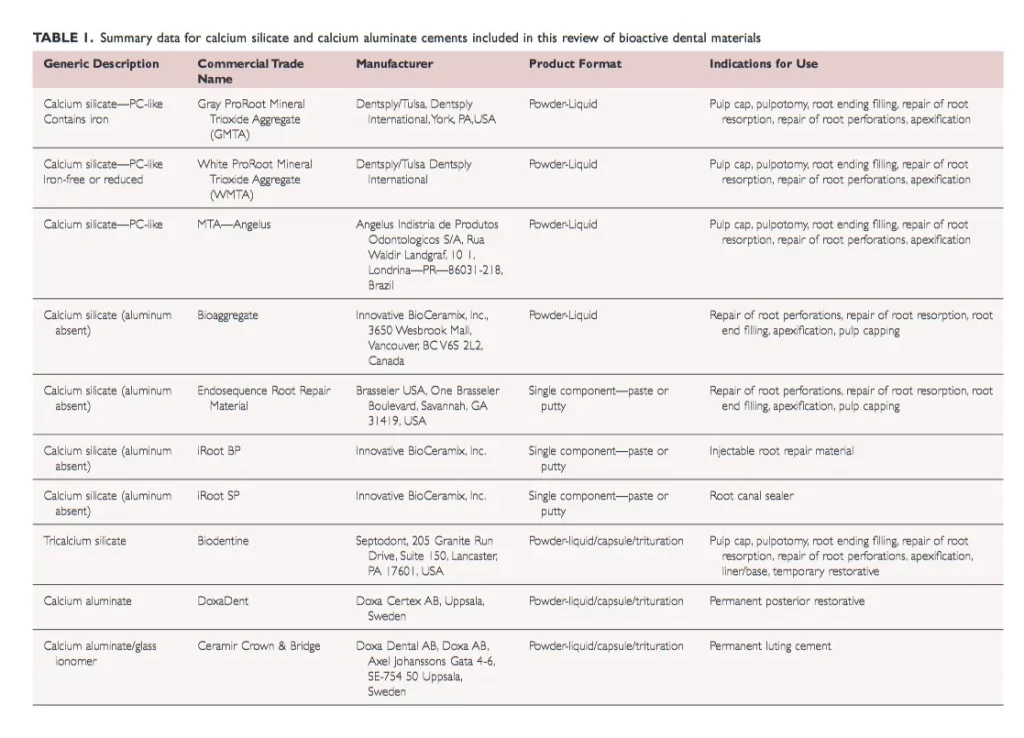
Primarily we have calcium silicates and calcium aluminates but the bioactive dental materials often contain some mixture of both. This only refers to the calcium releasing bioactive materials not the fluoride only materials.
- Calcium silicate materials similar to MTA (Portland cement)
- Calcium silicate with phosphate and without aluminum
- The calcium silicates with mostly tricalcium silicate
- Calcium aluminate (typically bioceramic cements have this)
- Calcium aluminate and glass ionomer
Bioactive Glass Ionomer
Our oldest bioactive material. Glass ionomer and resin modified glass ionomer absorb and release free ions of fluoride.
Specific bioactive dental materials by trade name
Many of these materials are very similar. I am not including those materials in the table above.
- ACTIVA (Pulpdent) comes as both a filling and liner
- Beautifil (ShofuDental) comes as restorative filling material
- BioCem (NuSmile) this is the exact same as ACTIVA cement and I heard just repackaged for NuSmile.
- TheraCal LC (BISCO) is a dental liner
- Biodentine filling
Bioactive Cements
- Theracem
- Activa Bioactive
- Ceramir
- Biocem Universal
Bioactive Liners
- Activa
- Biodeninte
- CaOH Dycal and Lite
- TherCal LC
- Limelite
- MTA
MTA mineral trioxide aggregate
MTA was the bioactive dental material that jump-started the interest in the field. It consists of portland cement 75%, bismuth oxide 20%, and gypsum 5% and trace amounts of silicon dioxide, calcium oxide, magnesium oxide, potassium sulfate, and sodium sulfate. Portland cement is tricalcium aluminate, dicalcium silicate, tricalcium silicate, and tetracalcium aluminoferrite. The removal of tetracalcium aluminoferrite removes the gray color and creates White MTA.
Information about some bioactive dental materials
TheraCal is in a new class of materials called resin-modified calcium silicate RMCS.
MTA Fillapex is resin base endodontic sealer and is similar to Fillapex MTA cement.
Biodentine by Septodent is a calcium silicate product. It is very similar to MTA with some improvements. Biodentine is made of tricalcium silicate, dicalcium silicate, calcium carbonate, calcium oxide, iron oxide, and zirconium dioxide as a radiopacifier. The liquid portion is calcium chloride and a polymer.
Activa Bioactive by Pulpdent is a bioactive cements that releases flouride, calcium and phosphate. I have been told that BioCem by NuSmile is actually made by someone else and the only other product availabe is Activa so….
MTA research for perforation
MTA beats biodentine in furcation perforation repair. Assed Bezerra Silva JOE 2017
MTA repair of perforations is successful in the short run but decreases dramatically over the long run. Initial healing is seen in 96% of cases but failure of the repair reaches 62% by year 14. Gorni JOE 2022.
TheraCal by Bisco
A light cure material made of tricalcium silicate cement and 45% resins. It’s all the similar resins as composite but also has polyethylene glycol dimethacrylate that allows mixing of resins and tricalcium.
Ceramir cement by Doxa
Ceramir is a hybrid material consisting of calcium aluminate and glass-ionomer components. It’s new and I’ve seen conflicting reports on whether or not it’s actually better in any way. Pameijer shows that micro-leakage of Ceramir is the same as Rely x luting plus in the short term. Ceramir does test higher than other cements for antibacterial properties. Unosson Of course the main reason we have interest in Ceramir is due to it’s ability to remineralize at the margin. Alhuwayrini However some tests show this does not actually happen. Dandoulaki JPD 2019 I agree with those tests as I have seen more crowns come off with ceramir and the cement is always on the crown not the tooth. It is testing as acceptable retention. Jefferies J Clin Dent 2009 Jefferies 3 year test
Bioactive dental liners
TheraCal LV by Bisco, Activa BioActive Base/Liner and Biodentine.
Giomer products
Giomer products have been around for a long time but Shofu’s new line of Beutifil products are nice and like all giomers release fluoride.
Bioactive dental material articles
Dental today article is very nice and so is this review article.
Other similar topics to bioactive dental materials
Bioceramic dental materials are under the umbrella of bioactive dental materials.
Bioceramic materials include alumina, zirconia, bioactive glass, hydroxyapatite, and resorbable calcium phosphates. They are chemically and dimentionally stable, biocompatible, and osteoconductive. Biocermic materials are non-corrosive, bioinert, bioactive, and biodegradable, soluble or resorbable.
Bioactive molecule delivery systems should be in own post since this is tissue engineering
Bioactive molecules are active signaling molecules that both initiate and maintain cellular responses. They are one of the basic principles of tissue engineering triad; those three being stem cells, scaffolds, and bioactive molecules. The challenges dentistry has in using bioactive molecules is that high concentrations can be toxic to cells, bioactive molecules have may have a short half-life, and maintaining a high enough concentration for the therapeutic time period.
Dentistry uses bone morphogenic protein BMP for bone grafting, well technically we use rh-BMP2.